PTSD/Trauma Treatment
Our Team

Charity

Ezra

Jen

Jenny

Jon

Lesley

Metz

Ryan

Saria
PTSD/Trauma
In Greek, Trauma means wounding. On an emotional level, trauma impacts people by shattering one’s sense of security, self and connection to others. On a biophysical level trauma rewires the brain to be primed for threat and fear processing (posttraumatic stress activation) and damages the body (studies show on several major health dimensions those with experiences of trauma are at far greater risk of health complications throughout life, resulting in decreased life expectancy). Trauma can also significantly damage a person’s desire and the ability for relationship connection and attachment.
Conversely, an incredible phenomenon of Posttraumatic Growth which has been studied for decades, shows that people who experience trauma can grow psychologically in ways that those who haven’t experienced trauma do not have the opportunity for. On dimensions of appreciation for life, personal strength, emotional intelligence, relationship support and satisfaction, & spirituality, those who have had symptoms of PTSD can live far fuller and happier lives than those who have not experienced a traumatic event.

Treating PTSD / Trauma
At Qualia, we pride ourselves in being Trauma Treatment Clinics. This means across our clinics we have clinicians who are experts specializing in Cognitive Behaviour Therapy for Trauma (CBT-T). We also have a thriving ongoing trauma education and supervision program, so our services will continually be leading-edge, innovative and professionally excellent. Declared by the American Psychological Association, National Child Traumatic Stress Network and many other professional leaders, CBT for treating Trauma and PTSD is well known as the Gold Standard – the very best psychological intervention – for the treatment of PTSD and its symptoms.
Incorporating emotion regulation skills, flashback management, insomnia and nightmare treatment, exposure to and reauthoring trauma narratives, as well as somatically oriented interventions – we provide evidence-based treatment that is proven to alleviate symptoms of PTSD. Further, we take you past treating trauma and into the use of interventions that promote and harness the power of Posttraumatic Growth. Through these interventions, clients experience relief of their PTSD symptoms, repair networks in the brain that prime posttraumatic stress responses, strengthen neural plasticity, increase posttraumatic growth and reauthor the narrative of their lives.
For children and adolescents, we also focus on incorporating caregivers, creativity and age-specific posttraumatic growth activities.
Check out a Youtube video describing Trauma-Focused CBT https://youtu.be/m_nm5BZCRTo
Research showing the strength of CBT to treat PTSD
Studies specifically targeted at documenting CBT, cognitive behavioural therapy for trauma treatment and brain development have demonstrated the following:
- Youth receiving trauma-focused CBT saw a symptom reduction of 64% on MRI scans, specifically decreasing fear responses and activation in the amygdala
- A meta-analysis of post-partum/perinatal psychiatric conditions including trauma-related disorders proved CBT to be significantly effective in decreasing post traumatic stress disorder symptoms on brain imaging responses
- Studies of those with traumatic brain injuries have shown CBT interventions six weeks after injury to successfully decrease symptoms of PTSD at three and six months follow up, as well as decreases in distress and depression
- Neuroimaging results show significant decreases in depersonalization and derealization symptoms of adolescents with PTSD, following 20 weeks of Trauma-Focused CBT.
- Neuroimaging results of women who experienced abuse and then received Cognitive Trauma Therapy showed enhanced efficiency of neural responses to emotional events and reduction of prefrontal cortex and amygdala fear responses
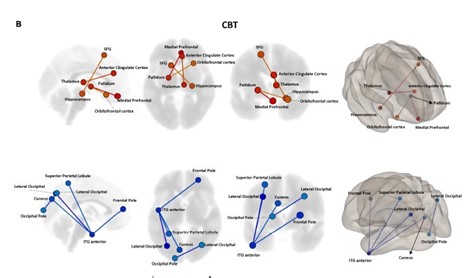
- Neural connectivity was shown to decrease for negatively impacting symptoms and increase for post-traumatic brain growth connectivity following trauma-focused CBT.
- Many studies have shown that neurocirculatory models through brain scan imaging improve significantly following trauma-focused CB, cognitive behavioural therapy treatment.
Who is at Risk of PTSD, Post Traumatic Stress Disorder?
In Canada, approximately 76% of people experience a traumatic experience in their lifetime with 20% of those developing PTSD. Post Traumatic Stress Disorder (PTSD) has about an 8% prevalence in the adult population, with about 5-6% of men, and 10-12% of women experiencing symptoms of PTSD in their lifetime. In the mental health population, estimates that 75-90% of those struggling with mental illness have a history of trauma, which is often not the presenting issue or concern but contributes to it.
From a Canadian perspective, these groups are at higher risk:
- Female population – research shows that the brain shrinks more for females than males when undergoing traumatic stress which results in worse long term impacts
- Indigenous & Indigenous women – high prevalence of historical trauma impacts with 55% experiencing abuse of some kind, and indigenous women 12-16 times more likely to be murdered than non-indigenous women (the greatest population at risk of homicide in Canada)
- Immigrant and Refugee Population – estimates as high as 89% experience of trauma, depending on the country of origin (ex. Refugees from Cambodia had nearly 90% PTSD prevalence). Canada has a 20-25% immigrant and refugee population nationwide.
- Those who have been sexually assaulted/abused – are at higher risk of developing PTSD, with a prevalence of 65% of PTSD in this population
- Military / Armed Forces / Veterans – 30% increased risk
- First Responders, Police & Firefighters – 30% increased risk
- Health & Mental Health workers – studies show vicarious trauma present in anywhere from 5-45% of workers




How is PTSD experienced? What are the risks of not getting treatment?
- Intense emotion like horror, grief, fear, guilt or anger
- Distressing and intrusive memories or dreams of the experience or event
- Extreme distress in response to reminders (triggers) of the event
- Flashback memories of the event, including a disconnect from the present moment
- Physical symptoms like interrupted sleep/insomnia, heightened startle response, racing heart and anxiety/panic attacks
- Cognitive impacts like poor concentration, inability to focus or difficulty in learning new things
Long term, experiences of trauma have been associated with:
- Chronic suffering related to Post Traumatic Stress Disorder
- Ongoing heightened emotional reactivity, behavioural/violent outbursts/lashing out, impulsive and reckless behaviours
- Chronic comorbid disorders like substance addiction, depression and anxiety
- Acute and chronic disruption of learning and cognitive development
- Increased risk of suicide
- Decreased Life Expectancy
- Impaired Brain Development & Plasticity
- Chronic insomnia and sleep impairment
- Increased health risks and causes of death (related to mind body impacts)
